Do I need a scan? To scan or not to scan?
Are your scan results helpful or harmful?
One of the first questions patients ask us ‘Do you think I need a scan?’. The answer to this question isn’t straight forward and is dependent on many factors. Often, we can’t answer until a thorough history is taken and a physical examination possibly carried out. Those that aren’t asking are often the ones presenting with scans already in lieu, sometimes already distressed about their X-ray, CT, MRI or Ultrasound findings. Most of the time this stress is unwarranted, as scan reports are often full of scary medical jargon (good old “degenerative disc disease” springs to mind) which describe relatively “normal/age related changes“. There is a poor relationship between imaging findings and symptoms.
In the practice of Physiotherapy, we tend to not use scans as a means for diagnosis as they do not necessarily reflect the true problem or where/why pain is originating. Many people with no pain or injury can have abnormal findings on an US, CT or MRI.
So, the question is, when should a scan be ordered?
Pros for scanning
- Can be a great tool to rule in certain pathologies but just as importantly, to rule out sinister pathologies e.g. tumours (but guys, don’t worry, this is very rare!).
- Can tell us the severity of an injury and therefore influence further management. An x-ray for a severe ankle sprain can determine if there is a fracture, and if so a period of time immobilised in a boot or cast may be appropriate to allow appropriate healing
- Scans can confirm clinical findings which may suggest a specialist doctor review and possibility of surgery. An example is MRI for acute knee injuries. If clinical tests suggest an ACL rupture, an MRI can confirm this and along with a patients report of significant instability, a specialist doctor might feel surgery is required.
Cons for scanning
- Minor findings are of no value in helping to explain the majority of aches and pain. In fact, not only are they not helpful, studies suggest that they are even harmful from a psychological point of view especially when they tell the patient they have, disc diseases, arthritis and tendon tears.
- Some scans such as CT and X-ray do have radiation. While the dosages are low, radiation exposure is cumulative over a lifetime. Therefore, these types of scans should not be routinely ordered
- If you look, you will find! Scans will nearly always show ‘incidental findings’. These are findings which are not related to the current injury/symptoms and are quite common, however can sound awful and can lead to fear avoidance behaviours. Good examples from the info-graphic below are:
- 87% of adults between 20-70 with no neck pain have evidence of degeneration in the cervical discs in their neck.
- 96% of men between 40-70 years showed some sort of abnormality on shoulder scans.
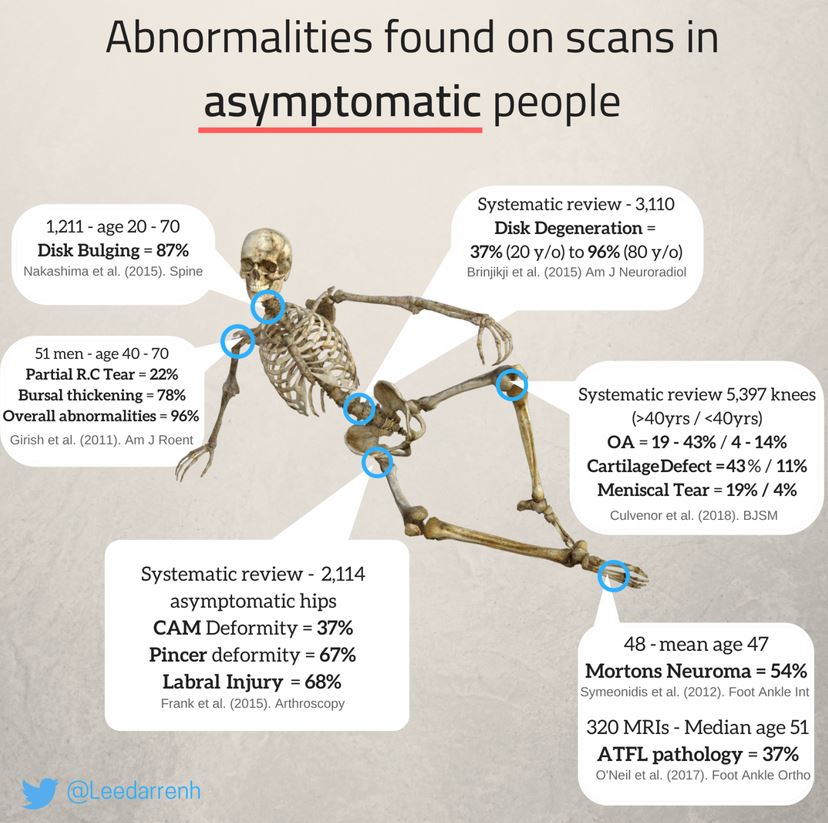
This is a fantastic infographic by Lee Higginbotham a summary of abnormalities found on scans in asymptomatic (no symptoms or pain) people.
When should I get a scan?
Scans in most circumstances’ are not needed in the first instance. A thorough clinical examination along with subjective history and mechanism of injury will help guide your physiotherapist. If the scan is not going to change the management then often they are not needed or can be done at a later stage if required.
If you do need a scan it is important that your physiotherapist or doctor takes time to go through the results and explains the result thoroughly. It is important they explain what findings are normal and abnormal and the best evidence based practice approach for you. Scans, when required and explained properly are very helpful however a lot of the time they over prescribed and poorly explained.
“WE TREAT PEOPLE, NOT SCANS”
Want to know more? Get in touch with our team at Mediphysio today
Thanks to Lee Higginbotham for the info graphic
https://www.ncbi.nlm.nih.gov/pubmed/25584950
https://www.ncbi.nlm.nih.gov/pubmed/21940544
https://www.ncbi.nlm.nih.gov/pubmed/25636988
https://www.ncbi.nlm.nih.gov/pubmed/25430861
http://bjsm.bmj.com/content/early/2018/06/09/bjsports-2018-099257
https://www.ncbi.nlm.nih.gov/pubmed/22835390
http://journals.sagepub.com/doi/abs/10.1177/2473011417S000311


Sorry, comments are closed for this post.