HAMSTRING INJURIES
Hamstring Injuries; a common injury

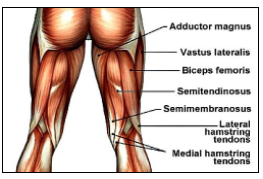
Hamstring injuries are the most common non-contact muscle injury seen in a variety of different sporting activities. We might hear in someone’s history, “I took off sprinting to get the ball and felt a pull in the back of my thigh” or “I went for a high kick and something just went pop”. There are two main types of acute hamstring strains that occur during different phases of running and kicking. Tears to the long head of biceps have shorter rehabilitation times and are most commonly torn at the musculotendinous junction, during activities such as high speed running (Brukner, 2015, p. 1241). Tears to the semimembranosus/semitendinosus parts of the hamstring are seen in movements with excessive lengthening such as dancing and require a longer rehabilitation time (Brukner, 2015, p. 1241).
Diagnosis of a hamstring muscle injury includes:
- pain on palpation
- pain on active muscle resistance
- decreased muscle length on passive straight leg raise testing (Mueller-Wohlfahrt et al., 2013)
In more severe cases of hamstring injuries, visible discolouration of the skin is evident due to a subcutaneous hematoma (bruises and contusions of the skin). As physiotherapists, we are well trained in diagnosing hamstring strains and are able to exclude all other differential diagnoses that can also cause posterior thigh pain (see table below).
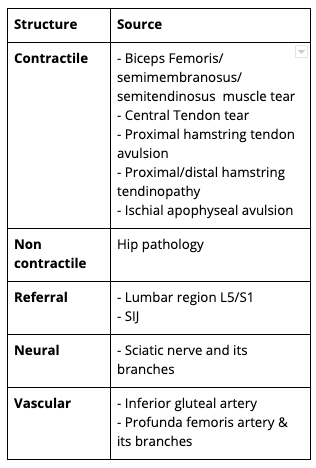
Predisposing factors and clinical grading systems
Predisposing factors associated with hamstring strains (Orchard, 2001):
- Age: Increased risk of injury as you get older
- Previous history of hamstring injury makes you 2-6 times more likely to re-injure
- History of lower back issues (L5 nerve impingement)
- Type of activity/sport: increased risk in sports involving sprinting, kicking and high speed skills
Clinical grading system:
Hamstring muscle injuries are graded based on the severity of the injury, in order to guide treatment and rehabilitation. This is based on clinical findings in the objective and subjective assessment. Imaging tools such as ultrasounds and MRI’s can be used to assist in grading the severity by measuring the length and cross sectional area of the muscle tear. However, imaging is most often not needed as a thorough initial assessment by a Physiotherapist can give a good guide of severity and injury prognosis.
- Grade 1 (Minor partial muscle tear)
- Grade 2 (Moderate partial muscle tear)
- Grade 3 (Subtotal muscle tear/tendon)
- Full proximal hamstring tendon avulsion: Needs a surgical review.
Some of these tears can be treated conservatively depending on factors such as age and activity levels. Proximal hamstring avulsions are commonly missed and can take 6 months to recover.
Treatment and Rehabilitation

After an accurate diagnosis by a Physiotherapist, rehabilitation can commence and is broken up into five phases focussing on muscle tissue repair and functional recovery. The goals of rehabilitation are to return to activity at pre injury function levels and to prevent re- injury (Mendiguchia, 2017).
- Phase 1: Promote healing, decrease pain and swelling.
- Phase 2: Restore range of motion, early optimal loading and minimise atrophy.
- Phase 3: Increase muscle loading, lumbopelvic control exercises, increase gluteal and hamstring strength.
- Phase 4: Introduce eccentric (lengthening) hamstring exercises as soon as able and progress to advanced lumbopelvic stability exercises.
- Phase 5: Introduce plyometric exercises and return to sport/running/agility program.
Patients are able to progress to each phase based on clearing a set criteria of outcome measures outlined by a Physiotherapist.
MANUAL THERAPY
Manual therapy techniques that can be used by Physiotherapists throughout the rehabilitation process include:
- Soft tissue massage of the hip flexors, erector spinae, adductors, gluteals, plantar fascia, hamstrings and calf
- Trigger point dry needling
- Lumbar spine mobilisations
- Muscle energy techniques
- Neural glides
PHYSIOTHERAPY MANAGEMENT The most recent guidelines for conservative management of a hamstring injury consist of:
ACUTE (PEACE):
- PEACE: Protection, Elevation, Avoid NSAIDs, Compression, Education
- Protect: De-load for 1-3 days but don’t completely rest, in order to preserve muscle strength
- Education: Reassurance, pain management and the importance of active recovery
- Avoid NSAIDs– studies suggest that it may be harmful in the acute stages of muscle recovery (Rahusen, Weinhold & Almekinders, 2004)
- Compression: Tubigrip or taping to decrease swelling
SUB-ACUTE (LOVE):
- LOVE: Load, Optimism, Vascularisation, Exercise
- Muscle loading through active range of motion and isometric exercises: encourage early muscle activation, reducing scar tissue build up and avoiding muscle atrophy
- Optimism: Identify fear avoidance and encourage positivity
Check out the Nordic drop rehab video below, a common rehab exercise prescribed for higher level hamstring loading. Have a chat with our team today if you wish discuss hamstring rehab further.
References: -Brukner, P. (2015). Hamstring injuries: Prevention and treatment—an update. British Journal of Sports Medicine, 49(19), 1241-1244. doi: 10.1136/bjsports-2014-094427 – Mueller-Wohlfahrt, H., Haensel, L., Mithoefer, K., Ekstrand, J., English, B., Mcnally, S., . Ueblacker, P. (2013). Terminology and classification of muscle injuries in sport: The Munich consensus statement. British Journal of Sports Medicine, 47(6), 342-352. doi: 10.1136/bjsports-2012-091448 -Orchard, J. (2001). Intrinsic and Extrinsic Risk Factors for Muscle Strains in Australian Football. The American Journal of Sports Medicine, 29(3), 300-303. doi: 10.1177/03635465010290030801 -MENDIGUCHIA, J., MARTINEZ-RUIZ, E., EDOUARD, P., MORIN, J.B., MARTINEZ-MARTINEZ, F., IDOATE, F., MENDEZ-VILLANUEVA, A. A Multifactorial, Criteria-based Progressive Algorithm for Hamstring Injury Treatment, Medicine & Science in Sports & Exercise: July 2017 – Volume 49 – Issue 7 – p 1482-1492 doi: 10.1249/MSS.0000000000001241


Sorry, comments are closed for this post.