Lower limb injuries in children

THE IMMATURE ATHLETE
At Mediphysio we work so closely with GPs and this allows us to see all kinds of conditions that come through the medical centres. Like a GP we often end up treating whole families, the mum, the dad and even their children as they go through their varying activity levels, growth spurts and potential injuries.
Our kids
Participation in youth sports and activities are popular and widespread in Australia. Maybe it’s due to our amazing weather that makes outdoor sports so enticing. The enthusiasm of children will often lead them to trying their hand at multiple sports at the same time, from swimming to touch football or basketball. With the addition of each sport they may start adding different yet cumulative stresses on their body.
Various unique factors, such as skeletal, psychological and emotion immaturity, underdevelopment of coordination, and unique response to skeletal injury must all be considered when managing injuries for this population.
THE ACTIVE YOUTH
The bones of children and adolescents possess a special area where the bone is growing called the growth plate. Growth plates are areas of cartilage located near the ends of bones. When a child is fully grown, the growth plates harden into solid bone. Some growth plates serve as attachment sites for tendons, the strong tissues that connect muscles to bones such as around the knee and ankle.
Highly active youths around early puberty, 8-13 years for girls and 12-15 years for boys, are prone to several conditions that only affect the developing skeletal system. These tend to include the apophyses ( normal developmental outgrowth of a bone, which arises from a separate ossification centre) , such as those at the knee (i.e Osgood-Schlatters Disease) or hip (traction aphophysitis at the ASIS) and Osteochondroses such as Perthes’ Disease.
Some clinical features of common lower limb conditions
Osgood-Schlatters Disease (OSD):
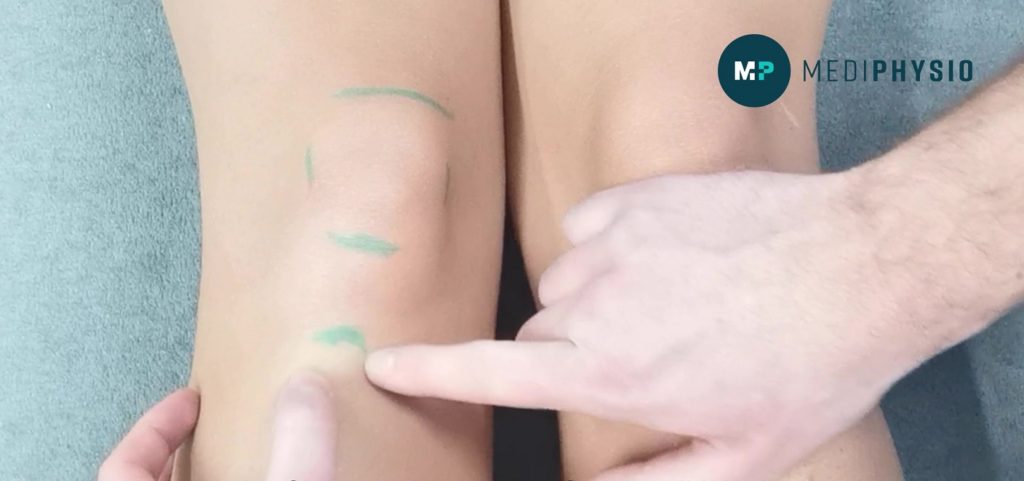
- apophysitis of the patella tendon into the tibial tuberosity
- most common
- localised tenderness +-swelling over the tibial tubercle
- insidious onset of symptoms
- often occurs around an increase of activity levels
- may lead to protruding tibial tuberosity if left untreated
Sinding-Larsen Johansson Disease
- apophysitis of the inferior pole of the patella and superior patella tendon
- similar to OSD, but less common
Severs Disease
- apophysitis of the Achilles insertion into the calcaneus
- reduced ankle dorsiflexion (bending)
Perthes’ Disease
- osteochondrosis of the femoral head
- age 4-10 years, with M > F
- low grade ache or limp
- restricted adduction and internal rotation of hip joint
Slipped Capital Femoral Epiphysis
- displacement of the femoral epiphysis relative to the femoral neck
- gradual or sudden
- presents with a limp; pain may also be in the knee
- reduced abduction and internal rotation
- may require surgical stabilisation
- complications: avascular necrosis
How do physios help our younger patients differently?
Health professionals have a critical role in guiding both young patients and their parents in the appropriate management of not just their symptoms, but also their developing views on the impact that physical activity can have on their lives. We explore this more in our next blog Lower limb injury management in children. We will also be sharing some common taping techniques we use to unload around the knee. STAY TUNED!
If you are requiring some guidance as to how better help your child stay active. Contact us and make an appointment to today!


Sorry, comments are closed for this post.